Periodontal Care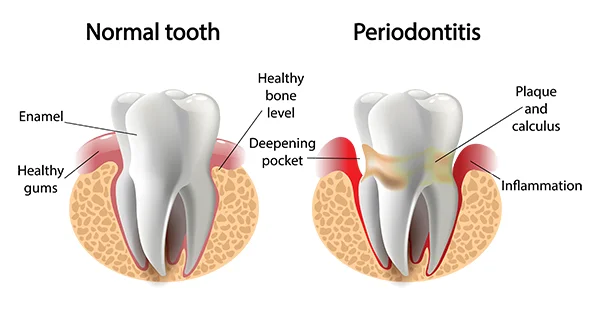 Periodontal maintenance is a crucial part of oral health that often goes overlooked. Periodontal disease affects the gums and supporting structures of the teeth. It is a common, but preventable condition that carries serious consequences when left untreated. Periodontal disease can be treated, and in some cases, reversed, but it requires diligent maintenance. Periodontal maintenance is a crucial part of oral health that often goes overlooked. Periodontal disease affects the gums and supporting structures of the teeth. It is a common, but preventable condition that carries serious consequences when left untreated. Periodontal disease can be treated, and in some cases, reversed, but it requires diligent maintenance.What is Periodontal Disease?Periodontal disease begins with the accumulation of plaque, a sticky film of bacteria, that forms on teeth. When it is not removed, plaque hardens into tartar. This leads to an inflammation of the gums called gingivitis. Without proper treatment, gingivitis may progress into periodontitis, a form of gum disease that can result in tooth loss, and larger health issues. The Importance of Periodontal MaintenanceRegular periodontal maintenance is essential to prevent progression of the disease. Maintenance allows for early detection of potential issues, and preservation of overall oral health. It is a basic part of maintaining a healthy smile, and prevents the systemic health problems associated with periodontal disease. Effective Periodontal Care TechniquesGood oral health habits at home, along with professional cleanings and check ups are the foundation of periodontal care. Daily Oral Hygiene PracticesWe advise that patients brush their teeth thoroughly twice per day, and floss daily to remove plaque and food particles between teeth. Professional CleaningsRegular dental check ups and professional cleanings are crucial to maintain periodontal health. During these visits, we remove plaque and tartar buildup, polish teeth to remove stains, assess gum health, and provide personalized strategies to improve oral hygiene. Scaling and Root PlaningFor patients with more advanced periodontal disease, scaling and root planing may be necessary. This deep cleaning procedure starts when we remove tartar and bacteria from below the gum line. The next step is to smooth the root surfaces to discourage further bacterial attachment, and to promote healthy gum reattachment to the teeth. Dietary ConsiderationsDiet plays a big role in periodontal health, oral health, and overall wellness. We recommend that patients limit sugary and acidic foods that can contribute to tooth decay, to consume foods rich in vitamin C and D to support gum health, and to stay hydrated in order to maintain adequate saliva production. Saliva neutralizes acids and washes away food particles. Advanced Periodontal TreatmentsIn cases of severe periodontal disease, more advanced treatments may be necessary:
The Role of Technology in Periodontal CareAdvancements in dental technology have improved the diagnosis and treatment of periodontal disease. Digital X-rays provide more accurate and detailed imaging. Laser therapy provides a less invasive gum treatment alternative. Ultrasonic scalers provide more efficient plaque and tartar removal. Long Term Periodontal MaintenancePeriodontal health is an ongoing process that requires commitment and consistency. Patients who have undergone periodontal treatments require a strict maintenance schedule that often includes more frequent dental visits, and cleanings. Contact us at (860) 743-9032 to schedule your next periodontal maintenance and care appointment! |